America is facing a caregiver crisis, and one organization is helping come up with the solutions.
The New York-based non-profit Paraprofessional Healthcare Institute (PHI) is working to improve the lives of people who need home or residential care by improving the lives of the workers who provide that care.
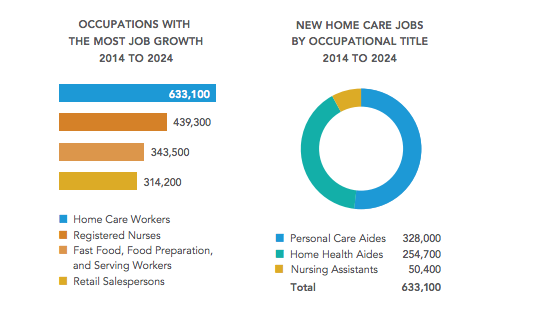
Americans are living longer than ever before. By 2050, the population of adults over the age of 65 is expected to almost double, growing from 47.8 million to 88 million. By 2024, home care occupations are projected to add more jobs than any other single occupation and is among the top 10 fastest-growing occupations.
Which is why developing a quality home health care workforce is so important. But that has been difficult due to do the lack of investment in home care workers.
The Numbers
- With a median hourly wage of $10.11 and work that is often part time or part year, home care workers earn on average $13,300 annually
- 1 in 4 (~24 percent) home care workers lives below the federal poverty line (FPL), compared to 9 percent of all U.S. workers
- More than half rely on some form of public assistance
This is where PHI is stepping in.
In addition to advocating for increased wages, PHI is also implementing advanced technology into their training programs to increase the skills of their trainees, helping prepare them for a 21st-century labor market, while giving them a strong sense of pride and confidence in their work and personal lives.
Care Connections Project
One of the innovative training programs PHI piloted in 2015, with funding from the New York State Department of Health, was the Care Connections Project (CCP).
For the project, the role of the Care Connections Senior Aides (CCSAs) was created to reduce preventable re-hospitalizations among clients of Cooperative Home Care Associates (CHCA) and Independence Care System (ICS), PHI’s affiliated managed-care agencies. Senior Aides work with home care workers in attending to and reporting unusual signs, symptoms or behaviors whose early detection could prevent a decline in health or the need for acute care. They also work with both clients and home care workers in the home in situations where unidentified or unaddressed issues threatened to “destabilize” the case.
To become a Senior Aide, trainees go through a three-month-long training program, including six weeks of classroom training and seven weeks of on-the-job training at ICS. During that time, aides enhance their observation and documentation skills, learn how to effectively offer other home care workers support and education, and deepen their knowledge of the chronic diseases that are most likely to lead to the preventable re-hospitalization of ICS members.
The sense of support and value aides feel in these new roles has resulted in increased confidence to be more ambitious and pursue further professional growth.
“I’ve been a home care worker for a long time,” said Beverly Harriott. “I love the work. It’s what I do. But my sisters always said it was a ‘dead-end’ job. Now I am a CCSA, and they don’t say that anymore.”
Senior Aides see a 60 percent wage increase, amounting to about $11,000 more per year than the average health care worker.
“It’s about creating rungs in the ladder, and developing the skills to climb that ladder,” says Angelina Drake, PHI Chief of Staff.

Marisol’s Story
Marisol Rivera wanted to be a health care provider because she enjoys helping people who need help. She trained for 200 hours to become a Senior Aide and now teaches fellow health care workers how to use the telehealth tablet. The tablet was designed to allow the caregiver to observe, record and report any changes to the client’s condition which alerts a nurse who can help with treatment immediately and possibly prevent hospitalization.
“Before it was back and forth, back and forth to the hospital — the majority of the time they would keep me in there,” says Althea Nelson, one of ICS’s clients. “With the tablet, it’s made it easier to communicate on a daily basis with a nurse so that things don’t go too far where I’d end up in the hospital.”
One time while she was training a caregiver at a patient’s home, Marisol noticed there was grit in the member’s catheter. “I asked about it and learned that the member couldn’t get to her appointment to get the catheter changed because the elevator was broken in her building. I informed my Clinical Manager, who was able to arrange to have someone come to her home to change the catheter, and this might have prevented a hospitalization for her down the road.”

In her new role, Marisol says she feels appreciated and respected by her peers, her supervisor, and the nurses she reports to. She says her children are very proud of her, especially her youngest.
Maribel Espinell-Quintero, Marisol’s clinical manager, says she’s seen a shift in how Marisol feels about the work she does since she started the program. She says Marisol’s become more outspoken, understands her role and how valuable it is.
“The responsibility that I have has given me more of a sense of being comfortable and confident in what I do,” Marisol says. “It has inspired me to continue my education, probably becoming an LPN or even an RN.”
What’s Next
In February 2017, PHI began identifying the most pressing policy issues facing direct care workers with the launch #60CaregiverIssues, a national, online public education campaign to tackle the growing crisis in paid caregiving.
“Our campaign is intended to deepen the public conversation on caregiving,” says Robert Espinoza, PHI Vice President of Policy. “We want policymakers, long-term care leaders, consumers, and the public to take this opportunity to learn about the issues, to share their experiences, and to join together to propose solutions that work.”
Over a two-year period, the campaign will release a new issue every two to three weeks, addressing five themes:
- Facts and Trends. What does the latest research say about occupational trends and the staggering mismatch between supply and demand?
- Future of Long‐Term Care. In many states, long-term care is being delivered through managed care organizations. What should we know about how this impacts the quality of jobs and quality of care?
- Quality Jobs. How do direct care worker wages compare to other occupations? What factors, beyond wages and benefits, impact the ability of employers to attract and keep these workers?
- Stories from the Field. Nearly 5 million direct care workers currently support over 8 million older Americans and people living with disabilities. Who are these workers, and who are the people they support? What can we learn from these stories about improving our systems of care?
- Training and Advanced Roles. Are a few weeks of training for direct care workers sufficient to meet the needs of millions of consumers living with physical disabilities or with conditions such as dementia?
“All of us will one day grapple with the challenges of finding accessible long-term care, either as a caregiver, someone managing care, or someone who needs care,” says Espinoza. “This is truly a universal problem.”